The rapid expansion of Medicaid managed long term services and supports (MLTSS) and other efforts to integrate healthcare and long-term services and supports is creating new, exciting and yet challenging opportunities for CBOs seeking to work within these new program designs. These new approaches mean that CBOs need to think differently about the services they offer, the customers they serve, and the way they demonstrate the value they add to services and supports. Instead of contracting directly with government funders, CBOs are now negotiating contracts with hospitals, health systems, accountable care organizations (ACOs), health plans, and other integrated care entities.
To understand the needs of the disability network community, the HCBS Business Acumen Center conducted an environmental scan of the business acumen of the disability network from April 2017 through May 2017.
Responses were solicited from the following three categories, each with its own unique survey:
- Community Based Organizations (CBOs).
- Managed Care Organizations (MCOs), Accountable Care Organizations (ACOs), and other healthcare and long-term services and supports payers.
- States currently operating or planning to implement a managed long-term services and supports (MLTSS) program.
See the categories below to view highlights from the environmental scan results:
| Who Responded to the Environmental Scan | Familiarity with Integrated Care Terminology | Experience Working with Integrated Care Entities | Importance and Current Skill Level in Key Business Areas |
Who Responded
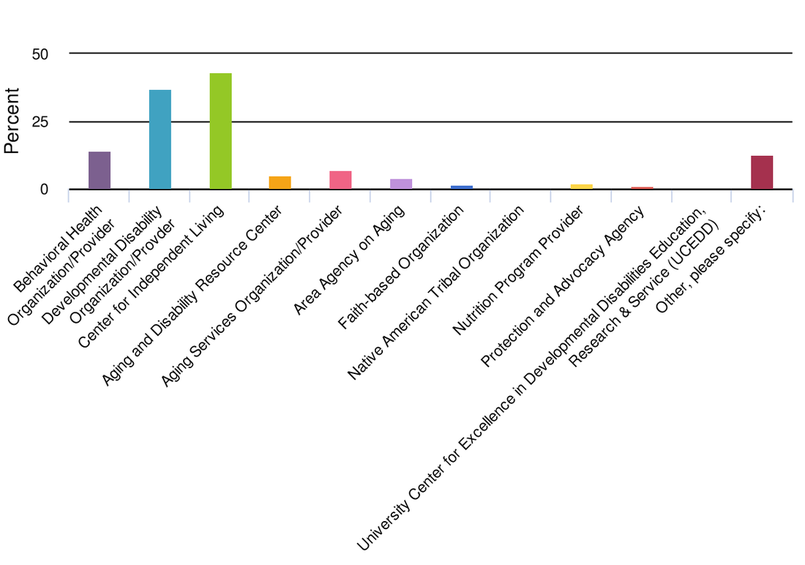
Of the 474 CBOs who responded, the majority or responses came from Centers for Independent Living, Developmental Disability Organizations and Behavioral Health Organizations. Please note that our target was disability organizations with some overlap with aging organizations. In addition to our resource center, there is another ACL funded business acumen resource center that focuses more on aging organizations. View the "Who Responded" bar graph displayed below in plain text.
 |
Familiarity with Integrated Care Terminology
How familiar are CBOs with integrated care terminology?
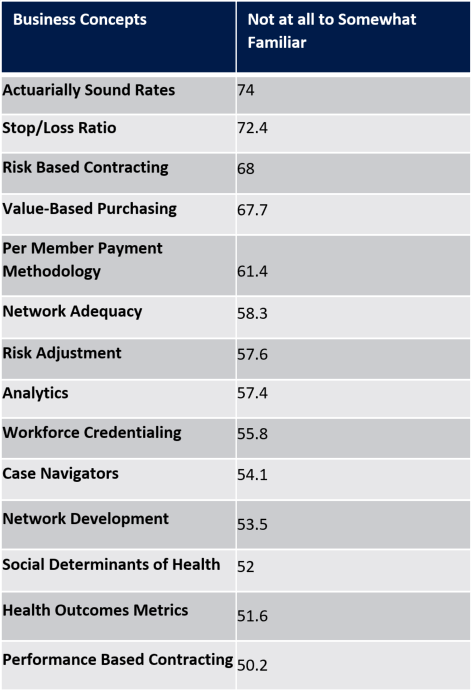
50% or more of the respondents were not familiar to somewhat familiar with the following concepts. View the "Familiarity with Integrated Care Terminology" table displayed below in plain text.
 |
To improve CBO familiarity in this area, we hosted a webinar entitled, "Are We Saying the Same Thing? The Language of Long-Term Services and Supports and Managed Care".
Experience Working With Integrated Health Care Entities
Do organizations have experience with contracting and negotiating with integrated care entities?
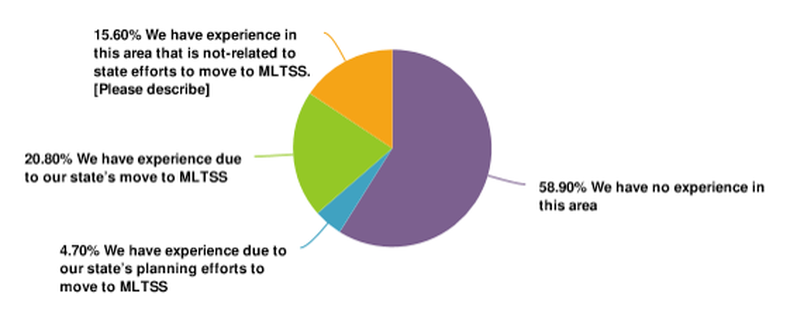
58.9% of CBOs reported that they have no experience contracting or negotiating with integrated care entities. View the "Experience with Contracting and Negotiating with Integrated Care Entities" pie chart displayed below in plain text.
 |
Has the shift towards MLTSS changed organizations capacity to provide services?
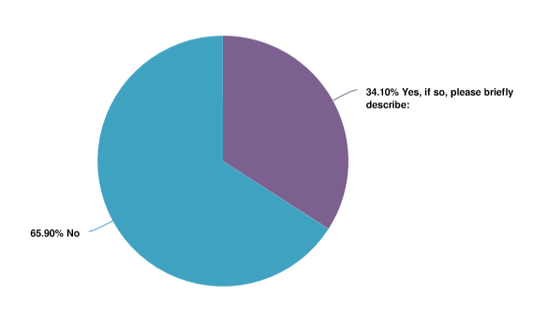
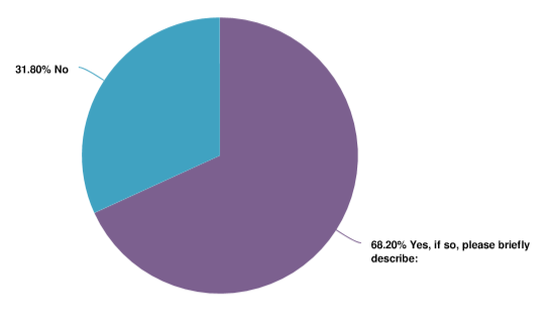
65.9% of Centers for Independent Living said that the shift towards MLTSS in their state did NOT change their organization's capacity to provide services; whereas 68.2% of Developmental Disability Organizations said that it did change their capacity to provide services.
- View the Centers' for Independent Living capacity to provide services with the shift towards MLTSS pie chart displayed below in plain text.
- View the Developmental Disability Organizations' capacity to provide services with the shift towards MLTSS pie chart displayed below in plain text.
| Centers for Independent Living: | Developmental Disability Organizations: |
 |
 |
Centers for Independent Living (CILs) reported that the shift toward MLTSS has helped them to build relationships with their managed care organization and build better supports for consumers with more complex needs. CILs are continuing to build capacity to contract with payers and providers, however, they continue to report concerns that the shift toward MLTSS causes actual and philosophical challenges due to attention on medical needs. Developmental Disability Organizations expressed concerns about changes in utilization, rates, and operational issues such as obtaining authorizations. However, they reported a desire to stay competitive and are willing to explore new opportunities to develop new services.
Importance and Current Skill Level in Key Business Areas
What factors contributed to unsuccessful attempts to partner with integrated health care entities?
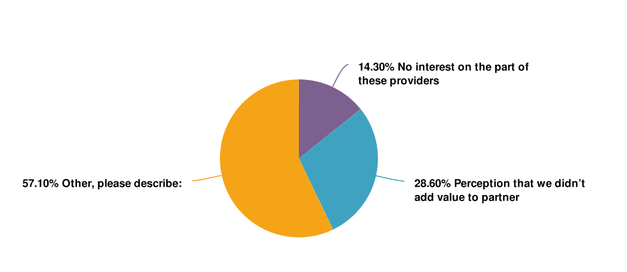
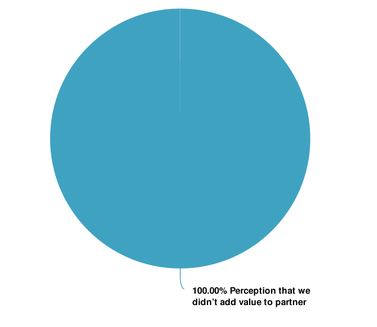
CBOs report that unsuccessful attempts to partner with integrated health care entities are often a result of the perception that they don’t add value to that organization and/or that they don’t have the data to substantiate their value.
- View the factors reported by Centers for Independent Living that contributed to unsuccessful attempts to partner with integrated health care entities pie chart displayed below in plain text.
- View the factors reported by Developmental Disability Organizations that contributed to unsuccessful attempts to partner with integrated health care entities pie chart displayed below in plain text.
| Centers for Independent Living: |
 |
| Developmental Disability Organizations: |
 |
To improve knowledge of how CBOs may maximize partnerships with health plans, we hosted a webinar entitled, "Are They Buying What You're Selling? An Inside Look at What Health Plans Need from Community Based Organizations".
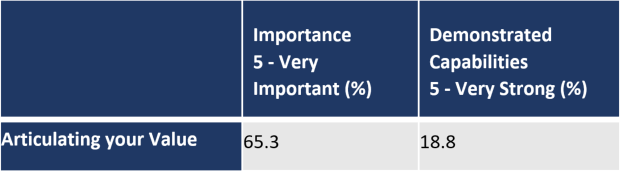
What are CBOs current skill levels in articulating their value?
65.3% of CBOs said that the ability to articulate their value to potential payers was very important; however only 18.8% said that their demonstrated capability to articulate their value was very strong. View the "CBOs Current Skill Levels in Articulating their Value" table displayed below in plain text.

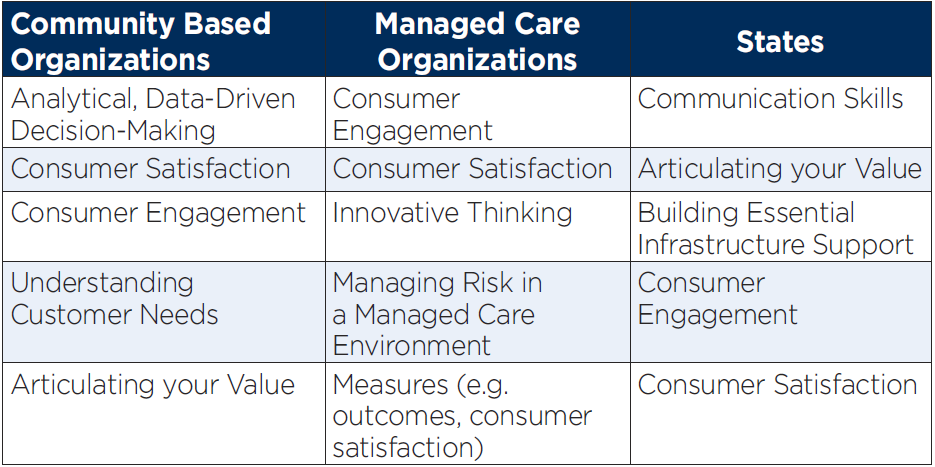
What skills and expertise did community-based organizations, managed care organizations, and states report as most important when modernizing the delivery of care and services? View the "skills and expertise reported as most important" table displayed below in plain text.